insights
What Is the IFM Toolkit?

Read Time: 3 Minutes
Functional medicine restores balance by strengthening the fundamental physiological processes of the body and adjusting the environmental inputs that nurture or impair them. This takes the form of therapies that focus on restoring health and function rather than simply managing signs and symptoms, which has been the traditional mode of medicine for centuries. This is an exciting time for the evolution of health care.
And yet, new paths are often fraught with trepidation. How can a healthcare provider transition into practicing functional medicine? What guides are available to help them along this path? This is where the IFM Toolkit comes in. The toolkit is a highly valued resource that is designed to assist practitioners in helping patients achieve their health goals. It contains hundreds of items, including:
- Patient assessments and questionnaires
- Intake forms
- Screening tools
- Lifestyle prescriptions
- Comprehensive food plan guides with weekly meal planners and recipes
- Patient education materials on nutrition and other modifiable lifestyle factors
- Clinical decision trees
- Protocols and condition-specific resources
- Translated tools in Spanish and Mandarin
The IFM Toolkit includes many resources that clinicians can use as patient education handouts, as well as several practitioner-specific resources about how to effectively practice functional medicine.
Explore the Newly Redesigned Toolkit
In 2021, IFM redesigned the layout of the toolkit according to practitioner feedback and best practices. The redesign of the toolkit represents our desire to innovate and improve on the educational materials and resources we offer, as well as to provide added value for IFM membership. Some of the improvements include:
- Intentional, intuitive curation to make it easier to find the resources you need
- Ease of navigation, with redefined categories
- Fillable PDF forms that allow you to type directly onto the document
- Improved keyword search efficiency
- Compatibility with desktop, smart phone, and tablet browsers
- A refreshed visual design
In the following video, you can explore the new features of the toolkit and preview select resources.
Examples of some of the most sought-after tools inside of the IFM Toolkit include the following:
Functional Medicine Timeline
One of the most popular toolkit items is the Functional Medicine Timeline. This tool allows practitioners to capture the patient’s important life events, family history, and genetic information from in utero to present day. In particular, the tool helps pinpoint antecedents, triggers, and mediators (ATMs) to help identify any role they play—past or present—in the patient’s disease. This foundational tool helps practitioners establish a therapeutic partnership with their patients and gives the space for each patient’s unique story to be heard and validated.

IFM Matrix
Functional medicine recognizes that illness does not occur in isolation, and the IFM Matrix helps practitioners examine the body systems, symptoms, and risk factors associated with a specific condition. The matrix provides an outline for the practitioner to organize the patient’s clinical imbalances in the following biological systems, called nodes: defense and repair, energy, biotransformation and elimination, transport, communication, structural integrity, and assimilation.
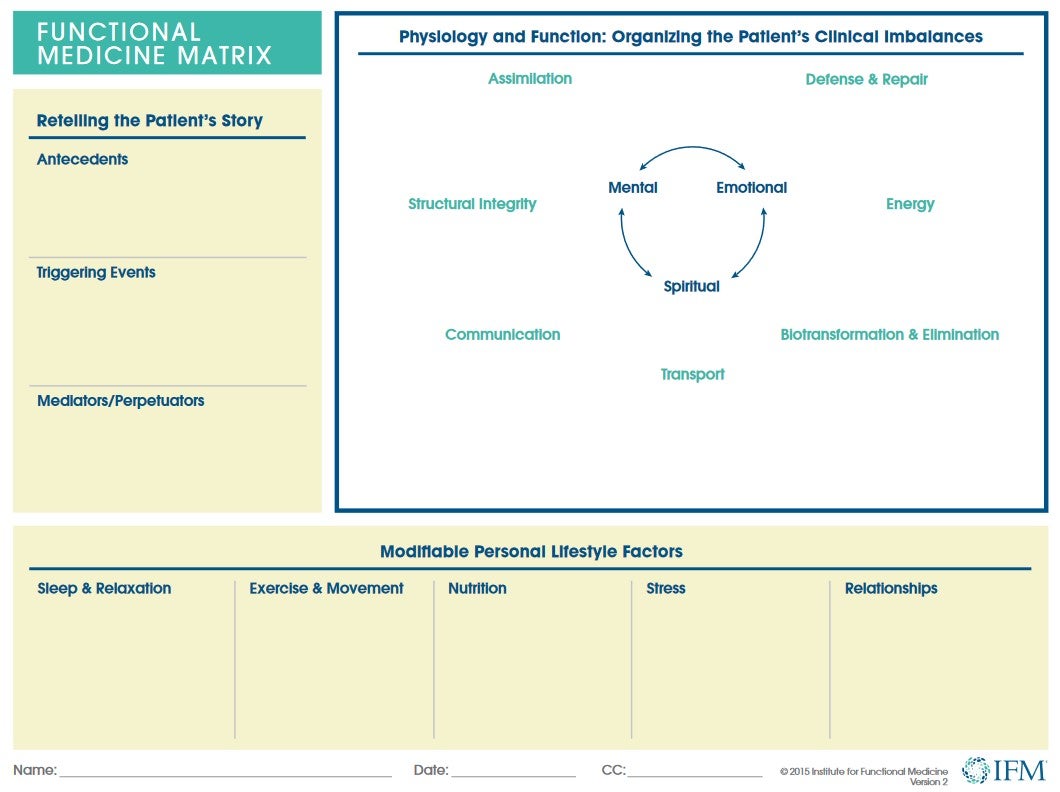
The left section of the matrix is useful in retelling the patient’s story by tracking antecedents, triggering events, and mediators/perpetuators. The bottom of the matrix details lifestyle factors like sleep and relaxation, exercise and movement, nutrition and hydration, stress and resilience, and relationships and networks.
As a whole, the Functional Medicine Matrix assists the practitioner in organizing and prioritizing each patient’s health issues as elicited through a thorough personal, family, social, and medical history. The matrix helps clinicians organize what may seem to be disparate issues into a complete story to help the clinician gain a comprehensive perspective of the patient and subsequently facilitates discussion of complex, chronic disease with the patient.
The IFM Toolkit is one of the most robust collections of functional medicine resources available to practitioners and offers a variety of dynamic, clinical resources to use in practice. IFM continually updates the toolkit resources with the latest evidence-based research and considerations. All practitioners who complete IFM’s premier course, Applying Functional Medicine in Clinical Practice (AFMCP), have access to the IFM Toolkit, which contains a wealth of information for new and seasoned practitioners alike.
With IFM membership, the toolkit can be accessed anytime. IFM members also receive the monthly Connections newsletter, which features a new or updated toolkit item and clinical commentary from IFM’s Director of Medical Education Dan Lukaczer, ND. The “Toolkit of the Month” feature highlights each tool’s clinical application, utility, and relevance for a variety of patient populations. Connections features other exclusive content for IFM members, including a monthly hot topic article with recent medical research and updates.




